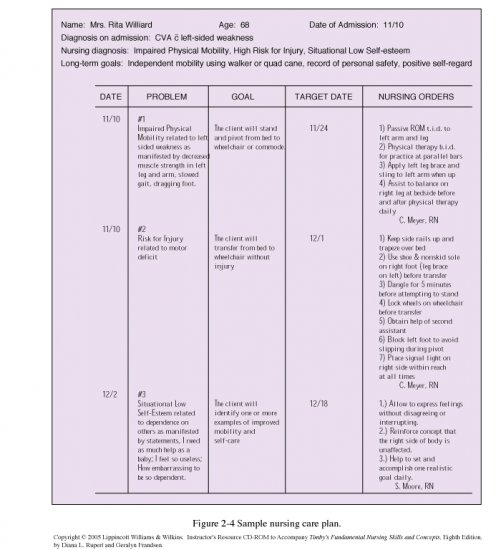
The client will have clear breath sounds to auscultation and will have respiratory status parameters with optimal air exchange.The client will achieve and maintain a patent airway.The client will achieve the normalization and ability to maintain patent airways and respiratory status.It is ultimately the nurse’s clinical expertise and judgment that shape the care plan to meet the unique needs of each patient, prioritizing their health concerns and priorities. In real-life clinical settings, it is important to note that the use of specific nursing diagnostic labels may not be as prominent or commonly utilized as other components of the care plan. While nursing diagnoses serve as a framework for organizing care, their usefulness may vary in different clinical situations. See nursing assessment cues under Nursing Interventions and Actions.įollowing a thorough assessment, a nursing diagnosis is formulated to specifically address the challenges associated with Parkinson’s disease based on the nurse’s clinical judgment and understanding of the patient’s unique health condition. 
Schedule regular follow-up appointments to monitor disease progression, adjust treatment plans, and address any concerns or changes in symptoms.Īssess for the following subjective and objective data:.Coordinate care and referrals to specialists, such as neurologists or speech therapists.Offer emotional support and counseling to patients and families to cope with the impact of Parkinson’s disease.Monitor for and manage potential complications, such as falls, dysphagia, or cognitive changes.Facilitate physical therapy and occupational therapy to optimize mobility, balance, and functional abilities.Provide support and education to patients and families about Parkinson’s disease, treatment options, and lifestyle modifications.Administer prescribed medications to manage symptoms, such as dopaminergic medications or anticholinergics.Monitor disease progression and assess motor and non-motor symptoms.Recognize and assess signs and symptoms of Parkinson’s disease.The following are the nursing priorities for patients with Parkinson’s disease: The nursing goals for clients with Parkinson’s disease include improving functional mobility, maintaining independence in performing ADLs, promoting safety and preventing falls, achieving optimal bowel elimination, attaining and maintaining acceptable nutritional status, achieving effective communication, developing positive coping mechanisms, and educating the client and their family on the disease process and self-care strategies to manage symptoms and improve the overall quality of life. With the introduction of levodopa, the mortality rate dropped by approximately 50%, and longevity was extended by many years (Hauser & Benbadis, 2020). These are resting tremors, rigidity, bradykinesia, and postural instability. There are four cardinal signs of Parkinson’s disease, with two of the first three required to make the clinical diagnosis. Initial clinical symptoms of Parkinson’s disease include tremors, subtle decrease in dexterity, decreased arm swing on the first-involved side, soft voice, decreased facial expression, sleep disturbances, rapid eye movement behavior disorder, decreased sense of smell, malaise, anhedonia, slowness in thinking (Hauser & Benbadis, 2020). The loss of dopamine stores in areas of the brain results in more excitatory neurotransmitters than inhibitory neurotransmitters, leading to an imbalance that affects voluntary movement. Neuronal pathways project from the substantia nigra to the corpus striatum, where neurotransmitters are key to the control of complex body movements. Parkinson’s disease is associated with decreased levels of dopamine resulting from the destruction of pigmented neuronal cells in the substantia nigra in the basal ganglia region of the brain. The disease affects more men than women and it’s the fourth most common neurodegenerative disease, with 50,000 new cases reported each year in the United States. 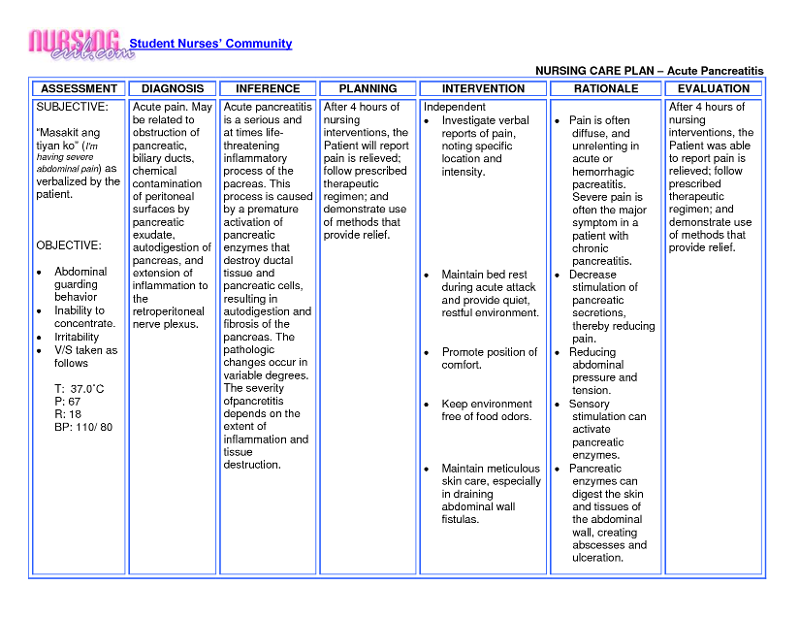
It occurs after the age of 50 and increases in incidence with age. 
Parkinson’s disease, or paralysis agitans, is a progressing neurological movement disorder that eventually leads to disability. Assessing and Monitoring for Potential Complications Monitoring Results of Diagnostic and Laboratory Procedures Administer Medications and Provide Pharmacologic Support Initiating Patient Education and Health Teachings Promoting Positive Coping and Providing Emotional Support Managing Dysphagia and Swallowing Difficulties Learn about the nursing assessment, nursing interventions, goals and nursing diagnosis for Parkinson’s disease in this guide. Use this nursing care plan and management guide to help care for patients with Parkinson’s disease.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
